Last year, at the end of a wonderful Valentine’s Day dinner in the hospital with my wife Amy, things took a turn again. A large object that looked like chicken fat was found in my ostomy bag. The nurses were very concerned and I was off for an emergency CT that evening. In the morning, I found out that several inches of my intestine wall were enlarged, but the physicians were not sure why. So, I was scheduled for a colonoscopy. But this was going to be very different, as I had no colon. An Ileostomy or a stoma is when the intestine comes out the front of the abdomen, about four inches to the right side of the belly button. In the GI lab, I chatted with the physician as he was getting the video equipment ready.
The flexible scope was small in diameter, much smaller than a colonscope. I requested no pain meds, as I wanted to be alert during the procedure. It was a very strange experience seeing a scope being inserted into your abdomen at the stoma (intestine). There was no pain or sensation of the scope, other than at the entrance at the skin. The images were fascinating to see and it was obvious were the problem was in the intestine. The inner walls of intestine were red and had a mucus look that was very different than the other areas. Biopsy forceps were used in one of the scope channels to take several samples of the inflamed tissue, I could not feel the forceps as they grabbed and pulled the tissue, but it did create a small amount of blood at the sample site. The physician was not completely sure what it was and would have to wait for the pathology report. Over the next several weeks, the tissue discharges in the ostomy pouch continued and my abdominal pain increased. The pathology reports came back clear for cancer and other disease, but indicated the tissue was ischemia, or dying from a lack of blood supply. This could be caused by a clot in the blood supply to the intestine, created back when I went into septic shock several days after surgery. The plan was to monitor it and see how it progressed.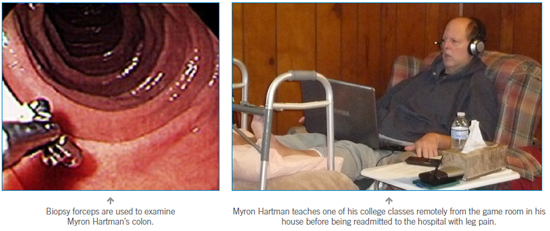
At the end of February, I was finally discharged from the hospital. My two months in the hospital had come to an end. I looked forward to coming home, but it was strange to be leaving the hospital. The nurses helped me 24×7 if I needed anything. I had a routine for meals, pills, dressing changes, physical therapy and my snacks in the evening. When at home I would need to make sure the walker could navigate the rooms, have my pills, dressings and supplies in place and I would now be on my own for attending to my ostomy bag. With the support of Amy and my family, I transitioned back home and started living in my new environment. When I went into the hospital in January, I had made plans with Penn State to return to the classroom in March. I had not accounted for the complications and my extended hospital stay. I could not drive and there was no way I had the strength and endurance to be back in the classroom. I talked with my supervisors at Penn State and decided that I would teach the spring medical equipment course from home through distance learning.
I had been using GoToMeeting.com for other Biomed Ed courses and had a good comfort level with it. The students were informed and the IT department at Penn State New Kensington set up the PC, projector and connection. About half of the students came into the classroom for the lecturers and the other half connected at home. As time went on, more and more students did go into the classroom for the interaction with the other students. For me, I used my laptop in the game room while in my recliner with all of my supplies by my side. I taught on Tuesdays and Thursdays from 9:30 a.m. to midafternoon. At the beginning, I would be exhausted after teaching. However, I think this helped me build up my endurance and strength. I had a web camera on me and there was one in the classroom so I could see the students. What appeared on my screen was projected on the screen at the front of the classroom. This was the next best thing to being there. I like to walk around talking with my hands and use the white board in a traditional classroom setting, so there were some changes to my teaching style. Overall, the classes went well and the feedback from the students was positive. This was somewhat of a test as well, as we have been talking about doing distance teaching at Penn State to other campuses for the program.
I continued teaching from home and then one evening in mid-April I had a cramp in my left leg. This was one of those cramps that would not stop. I tried drinking water, hot therapy, cold therapy, walking on it, pain pills, and anything else I could think of to stop the pain. This continued for over six hours and after seeking advice from my wife and doctor, I was taken to the hospital in an ambulance. After running some tests, they found I had three hematomas in my left leg. One of the arteries tore, possibly from the cramp, and bleed into the tissue in the upper leg. The leg was very swollen and sore. They did not want me moving around to prevent more bleeding. Being on blood thinners to prevent clots made this a challenge for the physicians. I was admitted to the ICU.
I had my wife bring in my laptop, headphones and the other materials I was using to teach. When class time rolled around, I connected to the hospital’s public Wi-Fi and class went on as scheduled. I sat up in my ICU bed giving the lecture as if I were at home in my recliner. One morning the physician team rounded while I was in the middle of a lecture. I told my class to take a break. The physicians asked what I was doing and I explained that I was teaching my biomedical engineering technology classes. They were amazed. One asked what the next subject was and said he may send over one of the residents to sit in on the class.
After five days in the ICU, I was moved to a general med-surg unit. Due to my limited movement to prevent bleeding at the hematomas, I developed a blood clot or deep vein thrombosis (DVT) in my left leg. So, I was back in bed with restricted movement to prevent the clot from going to my lung. I continued to teach my PSU classes during the day and my certification preparation courses for Biomed Ed in the evenings. The nurses were great at giving me the time to teach, as they would make their rounds as best they could not to disturb me while I was teaching. Some individuals could not understand my drive to teach and be active, but to me it was therapy and mentally stimulating. My faith, wife, family and a personal desire to become healthy again, all pushed me to remain positive, motivated and to return back to normal.
EDITOR’S NOTE: This is the sixth installment in a series of columns. The series began with a column in the December 2013 issue of TechNation. The columns can be found online at www.1technation.com.



