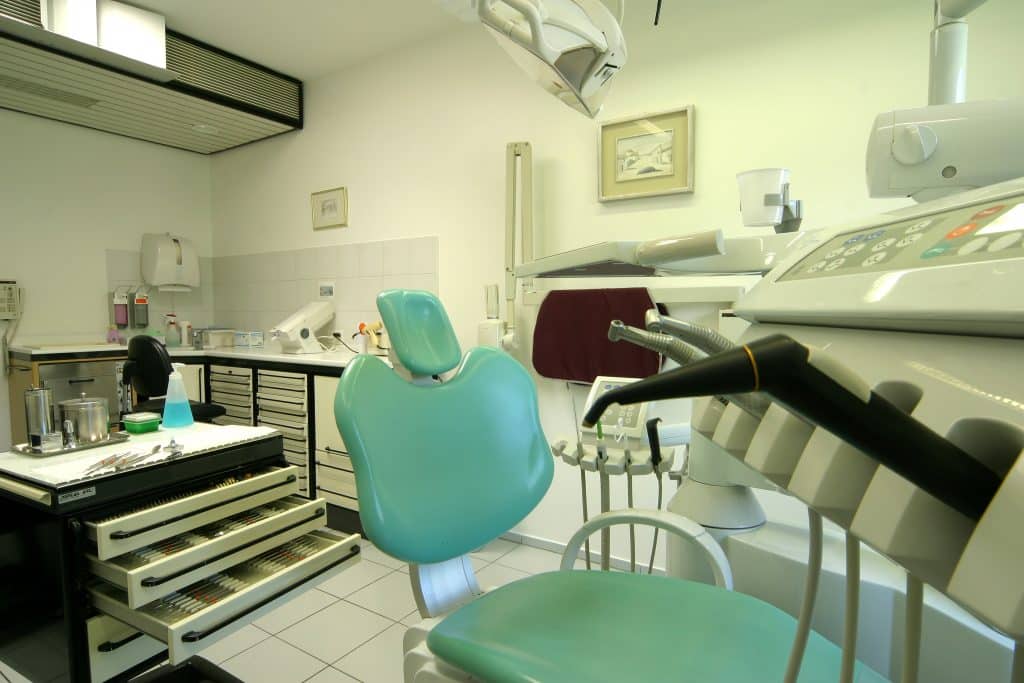
Several times in the 2009 American comedy film “The Hangover” Stu states that he is a doctor only to have it pointed out that he is a “dentist.” The gag plays on the belief many hold that a doctor is “not a real doctor.”
Yet, go to any dentist’s office and you will find medical devices and equipment that require regular maintenance and repair exactly like the medical devices found in urgent care clinics, hospitals and surgery centers.
The devices and equipment in dental settings continue to catch the eye and attention of more and more healthcare technology management (HTM) professionals – also known as biomeds.
One example of this growing attention to the dental sector was the 2024 UptimeHealth Dental Fix Summit in Nashville, Tennessee. It was supported by a popular provider of HTM education – the College of Equipment Technology.
The four-day event was designed “to equip independent dental equipment repair technicians and biomedical technicians with the latest technical training, business strategies, and networking opportunities in the dental industry.”
More recently, AAMI decided to spotlight the dental device and equipment sector of technology as this excerpt from a 2025 news release states: “UptimeHealth, a software and services company for outpatient healthcare, has built a strong presence in dental equipment management through its annual Dental Fix Summit. In a bid to bring that resource to the wider HTM community, AAMI has acquired the annual summit, with plans to make it a key feature of the association’s next annual HTM conference in Denver Colorado, May 29 to June 1, 2026.”
College of Biomedical Equipment Technology President Dr. Richard L. “Monty” Gonzales, an early proponent of the dental equipment management movement, noted that a biomedical equipment technician (or BMET) background provides a strong foundation for transitioning to dental equipment repair.
He pointed out that core competencies, including electronics, troubleshooting, mechanical and pneumatic systems, preventive maintenance, calibration, safety and infection control protocols, as well as imaging, sterilization and IT transfer directly to dental devices and systems.
However, much like a patient would not ask a primary care doctor to perform a root canal, hospital biomeds need additional education and training to service dental devices.
“These types of technical skills align with the proficiencies employers value and enable entry into many unique roles in the dental industry. Success in dental equipment service, however, necessitates targeted additional training,” Gonzales said. “Specialized components require focused expertise, including high- and low-speed handpieces, dental unit waterlines, advanced plumbing, amalgam separators, clinic-specific utilities, procedural workflows, and digital integrations distinctive to the dental environment. This specialized knowledge is typically acquired through original equipment manufacturer (OEM)-specific certifications or dedicated programs, such as those offered by the College of Biomedical Equipment Technology.”
However, there are many similarities especially when it comes to new technology.
“Mirroring the transformation and escalating technological complexity observed in traditional HTM roles – where networked devices, advanced imaging, and integrated software systems increasingly drive service demands – the dental sector similarly experiences robust demand fueled by the rapid adoption of digital dentistry technologies and ongoing needs for dental operatories,” Gonzales said. “Traditional equipment, such as high- and low-speed handpieces, dental chairs/treatment centers, air compressors, vacuum systems, and autoclaves, continue to generate high repair volume due to frequent mechanical wear and daily clinical use. Like the HTM industry, the dental industry demands timely maintenance and repair services.”
He added that biomeds have an advantage when it comes to expanding their services to include dental equipment saying it is “generally less complex than hospital-based medical devices, which feature advanced electronics, integrated software, networked connectivity with cybersecurity risks, and life-critical functions requiring rigorous calibration, electrical safety testing, and strict regulatory compliance.”
“In contrast, dental systems – such as chairs, delivery units, and autoclaves – focus on mechanical, pneumatic, and hydraulic components in compact, standalone setups with less emphasis on digital integration,” Gonzales said.
“However, dental equipment introduces unique challenges necessitating specialized training beyond standard BMET/HTM curricula,” he added.
The following is a Q&A where Gonzales shared more on this hot topic.
Q: What are the biggest challenges dental practices face in finding qualified service partners, and how can HTM professionals uniquely fill that need?
GONZALES: Dental practices face significant challenges in securing qualified service partners, primarily due to a severe shortage of specialized dental equipment repair technicians – with over 200,000 practicing dentists in the U.S. but only about 3,200 dedicated repair professionals – leading to reliance on expensive OEM services or delayed repairs. This scarcity is compounded by a prevalent tendency toward reactive maintenance, where practices often run equipment to the point of failure rather than investing in proactive care, resulting in costly downtime, appointment cancellations (potentially $500 to $2,000 per day in lost revenue), emergency repairs, and premature replacements that inflate overhead costs. Independent service organizations (ISOs) familiar with traditional HTM, as well as the experienced HTM professionals that comprise them, are uniquely positioned to fill this need – leveraging the training, experience, and lessons-learned in hospital settings to deliver reliable, cost-effective support tailored to the dental industry.
Q: Can you describe typical service and maintenance schedules in dental environments, and how they differ from those in acute care or ambulatory care settings?
GONZALES: In dental environments, typical service and maintenance schedules are heavily reliant on in-house staff performing daily tasks – such as flushing waterlines, cleaning handpieces, and sterilizing equipment – along with weekly or monthly checks for lubrication and basic inspections, while professional technician visits often occur only annually or biannually for calibration, part replacements, and deeper servicing. This contrasts sharply with acute care hospitals, where dedicated biomedical teams conduct rigorous, risk-stratified preventive maintenance quarterly or more frequently, strictly adhering to manufacturer guidelines and regulatory standards; ambulatory settings fall somewhere in between but generally feature more structured protocols than dental offices. The small, disparate, and often highly personal nature of dental practices – typically independent owner-operated offices scattered across communities – presents unique challenges, including limited dedicated maintenance staff and scheduling around patient care, compounded by narrow profit margins that make practitioners highly sensitive to repair costs, leading to a tendency toward reactive rather than proactive maintenance to control expenses despite the risks of downtime and equipment failure.
Q: How do regulatory, compliance and safety requirements within the dental market compare with those in hospitals and medical imaging departments?
GONZALES: Regulatory, compliance, and safety requirements in dental practices are generally less stringent and more decentralized than those in hospitals and medical imaging departments, reflecting the lower-risk outpatient nature of dental care compared to the high-stakes, life-critical environments of acute care settings. Dental offices are primarily regulated by state dental boards, typically with optional accreditation, and rely on manufacturer guidelines for equipment maintenance without mandatory centralized inventories or standardized preventive maintenance benchmarks. Although both dental and traditional healthcare sectors adhere to overlapping federal guidelines from agencies such as the FDA, CDC, and OSHA, the lighter regulatory framework in dentistry provides practices with greater flexibility, though it results in less uniform enforcement than the rigorously audited, compliance-driven hospital environment. Notably, the dental sector is seeing a growing emphasis on elevated quality and standards, driven in part by consolidation trends in which larger healthcare organizations and hospital systems are increasingly integrating, acquiring, or partnering with dental practices, bringing these offices under more comprehensive compliance frameworks and aligning them closer to traditional hospital-level oversight and safety protocols.
Q: What are some surprising benefits – business, financial, or professional – of working within the dental market, and how would you advise HTM professionals considering this step?
GONZALES: Surprising benefits of transitioning to the dental market for HTM professionals include tremendous business opportunities arising from a severe technician shortage – serving over 200,000 U.S. dental practices with only a few thousand specialized repair experts – creating fertile ground for independent service organizations, ISOs, or even entrepreneurship with high demand and growth potential in a projected 13% expanding field. Financially, compensation can be competitive or exceed traditional hospital BMET rates in certain regions, independent roles, or field service positions (averaging $60,000–$80,000+ annually, with outliers higher for experienced techs), while professionally, it offers diversification into a challenging, rewarding industry focused on unique equipment intricacies. I advise HTM professionals to pursue accredited dental-specific training, network at industry events like this year’s AAMI eXchange in Denver that will include an expanded emphasis on the dental sector, and start by partnering with local practices to build expertise – unlocking not just financial upside but also greater autonomy and job satisfaction in this underserved, vital sector.




